Mineral Bone Disease in CKD
Consequences of Mineral Bone Disease
Mineral Bone Disease (MBD), often seen in chronic kidney disease (CKD), is a major concern. As Delhi’s leading nephrologist, Dr. Debabrata Mukherjee offers expert care for managing CKD-MBD and related conditions.
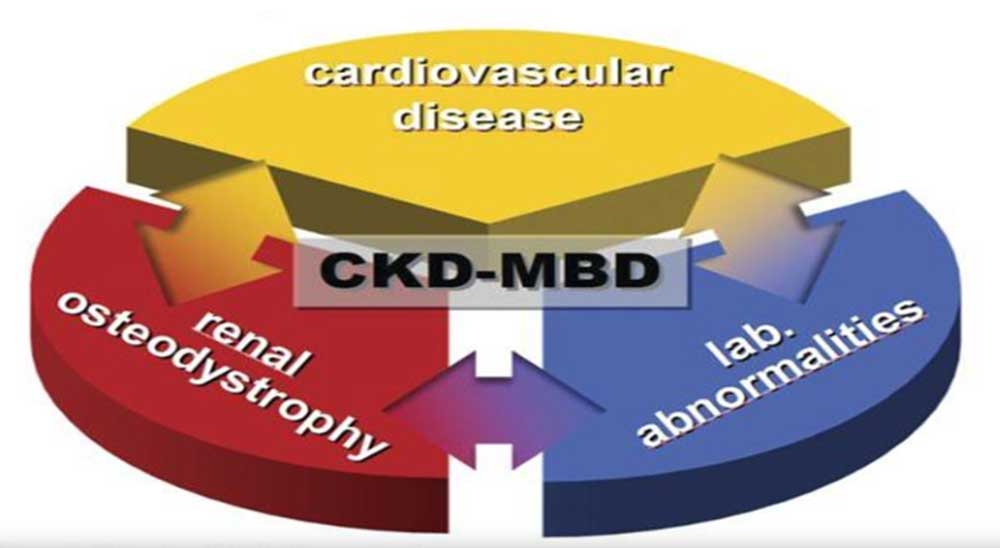
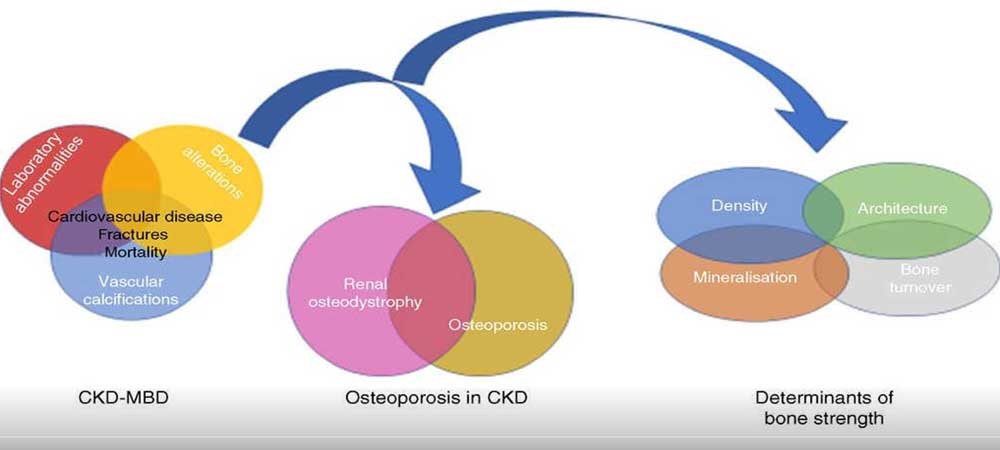
Common Consequences of CKD-MBD
- Bone abnormalities: Includes osteoporosis, osteopenia, and osteomalacia—causing fragile bones prone to fractures.
- Bone pain: Chronic bone pain reduces the patient’s quality of life.
- Fractures: Decreased bone density increases fracture risk even with minor trauma.
- Vascular calcification: Calcium deposits in blood vessels raise the risk of heart disease and stroke.
- Muscle weakness: Mineral imbalance affects mobility and increases fall risk.
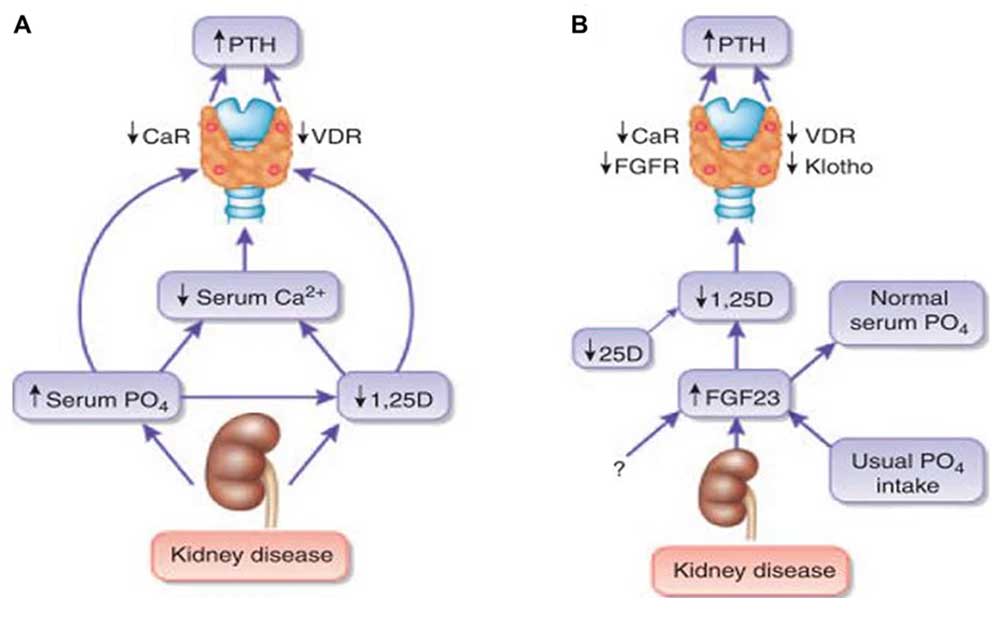
- Secondary hyperparathyroidism: Elevated parathyroid hormone (PTH) levels worsen bone loss and vascular damage.
- Renal osteodystrophy: A CKD-specific bone disorder resulting from disrupted mineral metabolism.
- Pruritus: Chronic itchiness due to elevated blood calcium and phosphorus levels.
- Increased mortality: Cardiovascular complications and fractures increase death risk in CKD patients.
- Reduced quality of life: Physical discomfort, pain, and psychological distress are common.
Effective Management of Mineral Bone Disease
Dr. Debabrata Mukherjee recommends a multi-pronged approach: managing mineral imbalances, prescribing bone-health medications, monitoring kidney function, and guiding lifestyle modifications.
Learn More from the Best Nephrologist in Delhi
- Kidney Disease Management
- Dialysis Services
- Renal Transplant Expertise
- About Dr. Debabrata Mukherjee
Contact Our Nephrology Expert
Email: dirnephro@gmail.com
For Appointments Contact: Co-ordinator at +91 9599471244

Prof (Dr) D Mukherjee is an alumnus of the prestigious Armed Forces Medical College, Pune where he did his MBBS & MD (Medicine). Subsequently he went on to do his DM (Nephrology) from PGIMER Chandigarh, which is the foremost training institution for nephrology in India.